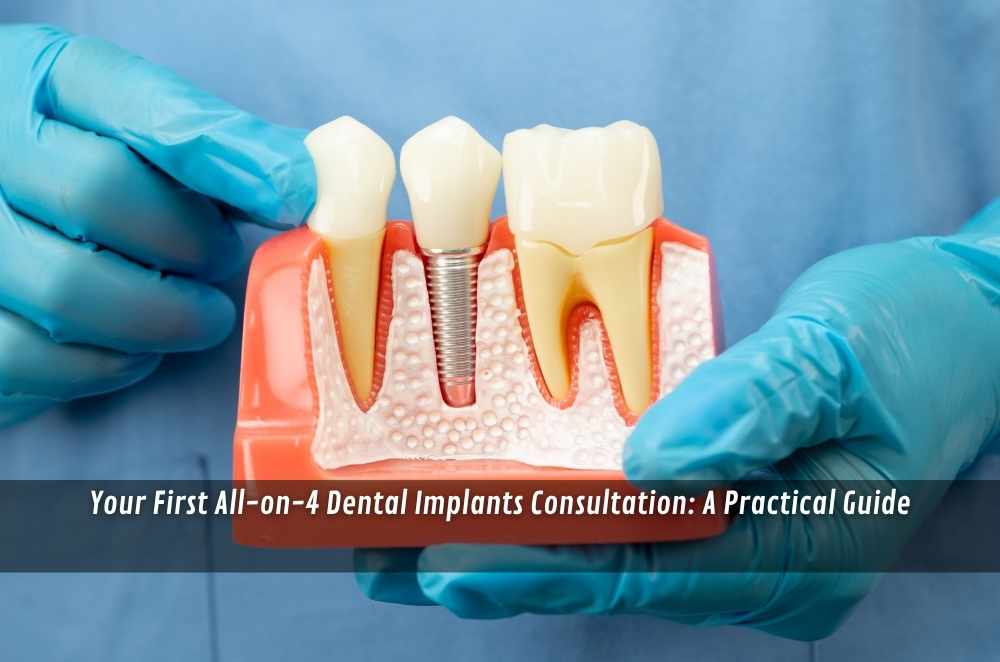
If you’re looking into full-arch implant options, the consultation can feel like the moment everything becomes “real”. You might have lived with loose dentures, failing teeth, or gaps for years — and now you’re being asked to make decisions about surgery, timelines, and what “teeth in a day” actually means in your situation.
A useful way to approach it is to treat the appointment as a planning session, not a sales pitch. The aim is to understand your health risks, your anatomy, and the trade-offs between speed, stability, and long-term maintenance.
To keep your preparation simple, here’s a established all on 4 dental implants consultation guide (High Dental Implants Melbourne) that outlines the kinds of assessments and planning steps many clinics include — like reviewing medical history, doing an oral exam, and taking X-rays or 3D imaging when needed. (High Dental Implants Melbourne)
What “All-on-4” usually means in real life
“All-on-4” is commonly used as shorthand for a full-arch implant approach where a fixed bridge is supported by a small number of implants (often four). But the label can hide a lot of variation: implant positions, whether implants are angled, whether extra implants are recommended, what materials are used, and whether the case is immediate-load or staged.
In other words, your consultation isn’t only about whether you “qualify” for a named technique. It’s about whether a full-arch plan can be designed safely for your bone, bite forces, gum health, and medical history — and what steps come first if something needs stabilising. (High Dental Implants Melbourne)
The core purpose of the consultation
A good consultation typically tries to answer four practical questions:
Is a full-arch implant solution appropriate for your situation?
What risks need to be managed first (infection, gum disease, medical factors)?
What does the likely timeline look like — immediate vs staged?
What will ongoing cleaning and maintenance realistically involve?
Many practices start by collecting a full medical history, doing an extra-oral and intra-oral exam, and then using imaging to plan implant placement (sometimes including CT/3D scans for more accurate assessment). (High Dental Implants Melbourne)
What clinicians assess and why it matters
Bone volume and bone quality
Full-arch bridges place significant forces on implants, especially when chewing tougher foods. That’s why imaging matters: it helps the clinician assess where bone is strongest and whether implant positions can be planned to support a bridge predictably.
A key point that’s easy to miss: bone loss doesn’t automatically mean you’re “not a candidate”. It often means the plan changes — sometimes with a staged approach, alternative implant distribution, or preparatory procedures when clinically appropriate. (High Dental Implants Melbourne)
Gum health and infection control
Active infection or uncontrolled gum disease can raise complication risk. In consults, this can lead to conversations about sequencing: stabilising gums first, removing teeth that can’t be saved, and planning around healthier tissue.
If you’re currently dealing with sore gums, recurring abscesses, or loose teeth, it’s worth asking how your clinic approaches infection control before implants are placed. (High Dental Implants Melbourne)
Bite forces, grinding, and clenching
If you clench or grind (especially at night), it may affect the early healing period and the design of the temporary and final bridge. This doesn’t always rule you out — but it may influence whether immediate loading is appropriate and whether protective measures (like a night guard) are recommended.
The consultation is a good time to bring up jaw soreness, headaches on waking, worn teeth, or a history of broken dental work — all clues that bite forces could be higher than average. (High Dental Implants Melbourne)
Medical history, medications, and healing factors
Implant treatment is still surgery. Clinics commonly ask about diabetes control, immune conditions, medications that affect bleeding or bone healing, smoking/vaping, and past healing issues after dental work.
If anything is complex, the safest outcome is often a plan that’s paced appropriately — sometimes with medical clearance or additional monitoring where needed. (High Dental Implants Melbourne)
Scans, records, and planning: what you might encounter
Depending on the clinic and your case, your appointment may include:
Clinical exam and photographs to assess gum health, bite, and smile aesthetics
Impressions or digital scans for study models and planning
X-rays and/or 3D imaging to map bone and anatomical structures
Discussion of options (including what happens if immediate loading isn’t suitable)
Some practices note that a CT scan may be recommended for more accurate planning, and may be performed onsite in certain settings. (High Dental Implants Melbourne)
If imaging is suggested, useful questions include:
What information are you looking for in the scan?
Does the scan change whether immediate loading is safe?
If you find limited bone, what are the plan B options?
Immediate teeth vs staged treatment: how to think about timelines
A lot of marketing collapses full-arch implants into a single promise: “teeth in a day”. In reality, timelines depend on stability, infection control, bone density, and bite risk.
A consultation should clarify:
Whether you’re a genuine candidate for immediate loading (a fixed temporary bridge early on)
Whether a staged approach is safer (healing first, then the bridge)
What “temporary” vs “final” bridge phases might look like
If a provider can’t explain why they recommend immediate or staged treatment for you, treat that as a signal to ask more questions (or seek another opinion). (High Dental Implants Melbourne)
The questions worth asking (and what the answers reveal)
“What makes me a good candidate — and what increases risk?”
You’re listening for specifics: bone findings, gum condition, medical factors, and bite forces — not vague reassurances.
“How many implants are you recommending, and why?”
“All-on-4” may be discussed as four implants, but some cases may warrant different numbers or distributions depending on anatomy and load planning. (High Dental Implants Melbourne)
“What does maintenance look like day-to-day?”
Full-arch bridges aren’t “set and forget”. You’ll likely need a daily routine to clean around and under the bridge, plus ongoing professional maintenance visits.
It’s reasonable to ask what tools people commonly use (e.g., soft brushes, under-bridge cleaning aids) and what warning signs to watch for (bleeding, swelling, persistent bad taste, discomfort on biting). (High Dental Implants Melbourne)
“What complications should I understand upfront?”
Any surgical or invasive procedure carries risk. A consultation should cover common complications and how they’re managed, in plain language, without minimising.
You can also ask what circumstances would lead the team to change course mid-plan (for example, if primary stability isn’t adequate for immediate loading). (High Dental Implants Melbourne)
“What happens if I’m not suitable for immediate loading?”
This is a great “reality check” question. A thoughtful answer often includes alternative staging, temporaries, or other restorative options — tailored to your situation rather than a one-size-fits-all pathway. (High Dental Implants Melbourne)
How to prepare before you walk in
A few simple steps can improve the quality of the conversation:
Bring a current medication list and relevant medical history notes.
Write down your top priorities (comfort, stability, speed, aesthetics, budget boundaries).
Note symptoms you may forget to mention (pain, swelling, loose teeth, grinding).
If you have old dental imaging or recent reports, bring them along (some clinics will review existing films when appropriate). (High Dental Implants Melbourne)
And if you feel pressured or rushed, it’s okay to pause. Complex treatment decisions benefit from time, clarity, and — when appropriate — a second opinion.
Key Takeaways
The consultation is best treated as a planning session focused on safety, suitability, and long-term maintenance.
“All-on-4” can vary between clinics; your anatomy and risk factors shape what’s recommended. (High Dental Implants Melbourne)
Imaging (including 3D scans in some cases) helps clinicians assess bone and plan implant placement more accurately. (High Dental Implants Melbourne)
Immediate loading (“teeth in a day”) is not universal; staged approaches can be the safer option for some patients. (High Dental Implants Melbourne)
Daily cleaning and ongoing maintenance are part of long-term success with full-arch implant bridges. (High Dental Implants Melbourne)

Write a comment ...